This article was originally handed in as a class assignment on Dec. 11, 2019.
Mayor Muriel Bowser’s multimillion-dollar plan to reduce opioid overdoses in Washington in 2020 has hit a major roadblock. Despite educational initiatives, Narcan distribution programs and increased efforts to combat fentanyl trafficking throughout the DMV, overdose deaths have not decreased this year, according to a report from the D.C. office of the chief medical examiner.
The D.C. government is fighting “a quiet storm,” said Chikarlo Leak, who tracks opioid overdose deaths for the medical examiner.
In a phone interview, Leak said the key factor contributing to the District’s continuing opioid crisis is a lack of trust in government institutions, leading to a high rate of death specifically in historically marginalized black communities in Washington. Although the city is working to sustain partnerships with local organizations, the rate of overdose deaths is stagnating.
The newest opioid overdose mortality report is not currently available online, but Leak said it shows overdoses are not declining despite the $24 million spent on reducing deaths in the District. The initiatives in place revolve around expanding education and awareness while also providing access to life-saving opioid reversal drugs like Narcan.
According to the 2019 second-quarter report produced by Leak Office of the chief medical examiner report, there are 14 fatal overdoses in the District every month. As of July 31, there were 98 opioid-related overdose deaths confirmed by the chief medical examiner compared to 109 deaths at the same time in 2018.
The Mayor’s plan
In order to address the increasing epidemic within the district, Mayor Bowser initiated the Live Long D.C. campaign in January 2018. The plan was implemented with the goal to cut opioid overdoses in half by 2020. The information provided by Leak casts doubt on whether or not this goal will be met by the end of next year.
“The District’s multi-stakeholder, public health approach has yielded progress in saving lives and reducing fatal overdoses,” the Mayor wrote in the strategic plan’s opening letter. “But there is still work to be done to reduce the impact of the epidemic on our city.”
The successes of the plan so far, according to Mayor Bowser’s letter, included reversing over a thousand opioid overdoses by distributing Narcan to community organizations, as well as monitoring synthetic opioids and providing educational materials on opioid addiction.
Between 2014 and 2018, 81 percent of all overdose deaths were African Americans, and 88 percent of all people who overdosed had been using for more than 10 years. This population provides a stark contrast to the average opioid user nationally, who are 18-29-year-old white men.
Live Long D.C. focuses on 7 goals, which include educating pharmacists and D.C. residents on opioid use, increasing access to harm reduction services and reducing barriers that might prevent or deter people from seeking out services.
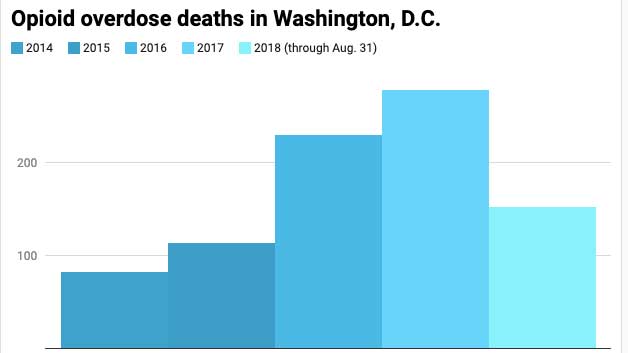
Although the rate of overdose deaths dropped by 31 percent between 2017 and 2018, according to Leak the number of deaths has not dropped between last year and this year.
Leak’s role includes looking for trends in mortality rates, assessing causes of death and creating special reports for the Mayor’s office. He also serves on the oversight board of the Live Long D.C. initiative. He uses this data to provide policy suggestions to the various government programs designed to reduce opioid overdose deaths.
In addition to producing mortality reports, Leak also participates in meetings with government officials to discuss ways to improve access to care services within D.C. The quarterly meetings allow Leak to discuss and review his reports in a way to address opioid use and addiction with the city’s government.
He said that building on community partnerships has been essential to reaching users who would not normally interact with government-operated care facilities.
Organizations like Bread for the City and HIPS, which provide a number of legal and health support services within Washington, are the center point for this goal. They provide Narcan to residents, offer syringe exchange programs to reduce the transference of disease and offer buprenorphine, which reduces withdrawal symptoms in individuals who are trying to stop using opioids.
The Mayor’s office did not respond to requests for comment on this story.
Deaths in the District
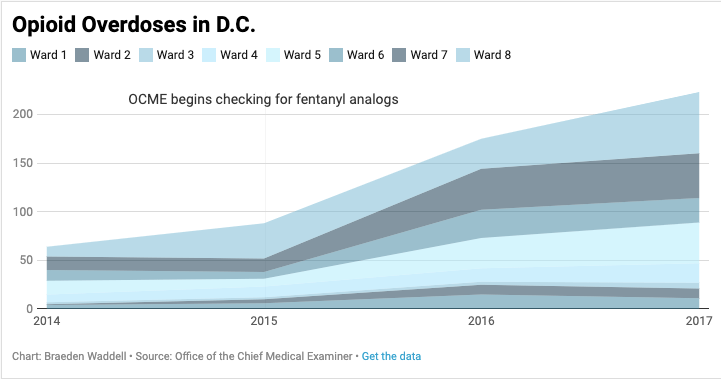
The 2019 report on overdose-related deaths shows Wards 5, 7 and 8 having the highest rate of overdose deaths. These neighborhoods are all predominantly black. African-American men between the ages of 50 to 59 are the most at-risk population for opioid-related fatal overdoses in the District, constituting nearly a third of all deaths in 2018.
Michael Kharfen, senior deputy director of the HIV/AIDS, Hepatitis, STD and TB administration for the D.C. Department of Health is in charge of the city’s Narcan distribution program, which was introduced earlier this year.
In a phone interview, Kharfen said that because the opioid-using population in the District is so different, the city’s response has been unique in the way it approaches providing services for substance users.
“Our first intervention effort was partnering with our needle exchange providers who have very long-standing relationships and rapport with people who have a longer-term use of drugs,” said Kharfen. “We were not necessarily applying the same toolkit that may have been applied in place that’s more rural, that has the younger users … or are using prescription drugs.”
Kharfen said that a key part of the city’s response to overdose deaths is understanding the relationship between the District’s using population and government support systems.
“[Washington] is very different in terms of where people are willing to access, whom they trust,” said Kharfen. “The distinctive approach in the District has been … partnering with the organizations that have that kind of credibility and authenticity with a community of people who’ve used drugs for a long time and have been often marginalized or rejected by other traditional systems of care.”
He said that while his goal is to provide better access to Narcan for family members and friends of drug users, he also thinks about “adopting and adapting to the needs” of the city’s unique conditions.
https://infogram.com/deaths-in-the-district-1hkv2nnx9epp2x3?live
Rana Bou-Serhal, the top pharmacist at an Adams Morgan neighborhood CVS that participates in the program, said her pharmacy has only distributed seven or eight kits since the program began. In 2018, there were eight opioid-related overdose deaths in Ward 1, where the pharmacy is located.
Bou-Serhal said “there’s no limit, they can get as many [kits] as they want.”
She said that she will then fill out a form that includes the requestor’s information as well as the number of kits they were given, which she then will fax to the Washington D.C. Board of Pharmacy.
Aside from the standard questions that pharmacists are required to ask, some local healthcare providers in the District go beyond the specific requirements laid out by the board of pharmacy.
Sukriti Kaushal, a pharmacist at Grubb’s Pharmacy Southeast, said in an interview that the pharmacy will cross-check a requestor’s name with their own database to view which medications they are currently prescribed.
“Any patient that comes in with a prescription that has the potential for abuse with the ability for Narcan to resuscitate, we offer them the Narcan for free,” said Kaushal.
She said the pharmacy offers patients information on the pharmacies that distribute Narcan, what days they’re open, and how to get to them. The pharmacy will also offer Narcan kits to friends and family members that pick up these prescriptions.
Kimberly Henderson, the director of communications and community relations for the D.C. Department of Health, said in an email that 1565 kits have been distributed since Aug. 31.
Purity and potency
Fentanyl is a highly potent synthetic opioid that is often cut into heroin in order to pack a more powerful punch in a smaller dose, making it easier to transport and distribute. This means that people who have been using opioids for decades are now facing an increased risk because it is nearly impossible to distinguish between heroin that is pure and heroin that contains fentanyl.
“You see a white powder, you don’t know the concentration” or purity of the substance, said Leak.
Leak said that his role on the Live Long D.C. advisory board includes making suggestions for policies that could reduce the number of overdose deaths involving fentanyl specifically.
“Handing out fentanyl test strips, getting Naloxone, and harm reduction” are all goals of the Mayor’s initiative, according to Leak.
In 2018, there were 213 total overdose deaths, with fentanyl contributing to 86 percent of fatalities. In the second quarter of 2019, 98 percent of all opioid-related overdose deaths in the District involved some amount of fentanyl.
Leak said that this trend remains the same for the unpublished third-quarter report.
Since the Office of the chief medical examiner first started testing for fentanyl in 2014, 873 of the 1,018 people who died from opioid-related overdose tested positive for the drug.
Despite this information, in the 24-page Live Long D.C. report published in March, fentanyl is only mentioned seven times despite accounting for well over 90 percent of all opioid-related overdose deaths. While the report mentions the prevalence of fentanyl-laced opioids, there is no specific plan to reduce fentanyl-related overdoses.
The only plan outlined in the report is to “develop effective law enforcement strategies that reduce the supply of illegal opioids in the District of Columbia.”
Leak said that continuing to focus on “implementing educational campaigns” will be the major factor in reducing opioid overdose deaths. In the coming months, bus stops and homeless shelters will have advertisements with information on how to get Narcan and begin addiction treatment at local facilities.
He said that “reducing regulatory barriers, creating a robust and comprehensive surveillance system, … supporting behavioral health programs and providing immediate access to intervention and care” are all key to reducing overdose deaths.
“We want to make sure residents and users are aware that there are services in the city,” said Leak.